研究成果 Research Results
- TOP
- News
- Research Results
- Miniature livers bioengineered from human stem cells able to function in rats
Miniature livers bioengineered from human stem cells able to function in rats
Advances bring lab-grown partial or complete organs for treating liver disease one step closer to reality 2020.06.17Research ResultsLife & Health
Fully functional miniature human liver grown in the lab.
Researchers from Kyushu University and the University of Pittsburgh have successfully transplanted miniature livers grown from human cells in the lab into rats. Bioengineered with multiple types of cells for full functionality, these mini livers demonstrated basic functions for four days after transplantation.
“Currently, the only cure for people with terminal liver failure is liver transplantation, but there are simply far too few donor livers available,” says Kazuki Takeishi, assistant professor at Kyushu University and co-lead author on the study announcing the new results in Cell Reports. “Thus, our dream is to be able to grow livers in the lab for transplanting into patients.”
To create the functioning mini livers, the researchers used a process that allows them to generate extremely versatile cells—known as induced pluripotent stem cells or iPS cells—from adult human cells and then reprogram these iPS cells for a job completely different than that of the original cells. In this case, they needed three types of cells: one for the main liver tissue, one for the vessels that distribute blood throughout the liver, and one for the bile duct that carries liver products to the intestine.
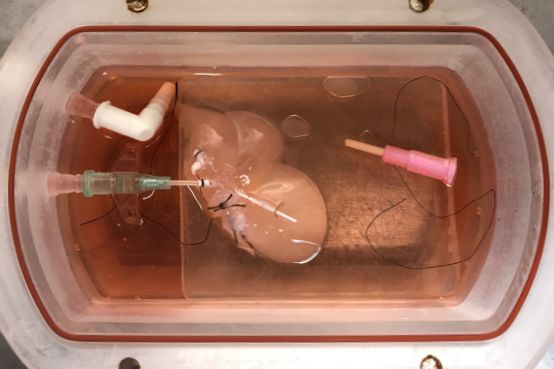
Scaffold used to organize cells into a miniature human liver.
Scaffolds to organize these different cells were made by removing all the cells from rat livers. After inserting the new cells into the scaffolds and letting them grow, the researchers transplanted the mini livers into rats, where the livers demonstrated basic functions such as metabolism and protein synthesis.
The prospect of being able to start from adult human cells poses major potential benefits in terms of organ compatibility. Even when people are deemed to be compatible for a transplant, suppression of the immune system is still necessary to prevent the body from rejecting a transplanted organ, opening the possibilities for additional health problems.
“Using this type of method, we hope to one day be able to engineer livers derived from a patient’s own cells, thereby providing an on-demand source of fully compatible organs that reduce the need for immunosuppression,” explains Takeishi.
Though the dream is one step closer than before, many issues still remain to be solved to scale up the mini livers and get them reliably functioning in humans, most likely first as a helper to the original liver instead of a replacement.
But whatever the challenges that may arise, Takeishi and his colleagues are determined to keep moving forward in their quest to bring relief to liver disease patients.
###
For more information about this research, see “Assembly and function of a bioengineered human liver for transplantation generated solely from induced pluripotent stem cells,” Kazuki Takeishi, Alexandra Collin de l'Hortet, Yang Wang, Kan Handa, Jorge Guzman-Lepe, Kentaro Matsubara, Kazutoyo Morita, Sae Jang, Nils Haep, Rodrigo M. Florentino, Fangchao Yuan, Ken Fukumitsu, Kimimasa Tobita, Wendell Sun, Jonathan Franks, Evan R. Delgado, Erik M. Shapiro, Nicolas A. Fraunhoffer, Andrew W. Duncan, Hiroshi Yagi, Tomoji Mashimo, Ira J. Fox, Alejandro Soto-Gutierrez, Cell Reports (2020), https://doi.org/10.1016/j.celrep.2020.107711
Research-related inquiries
Kazuki Takeishi, M.D., Ph.D., Assistant Professor
Department of Surgery, Kyushu University Beppu Hospital
Contact information can also be found in the full release.
- TOP
- News
- Research Results
- Miniature livers bioengineered from human stem cells able to function in rats